Research Article - (2018) Volume 8, Issue 4
Objective: To examine the effects of an integrated intervention program on the knowledge/skills, self-efficacy, and weight management practices among General Practitioners (GPs). Methods: A quasi-experimental (pre-and post-test) design was used. A convenience sample of 118 GPs from two community health services in Shanghai, China was recruited. The interventions included two 100 min training lectures with educational materials, including guidelines, brochures, and posters. Data were collected via self-administered questionnaires to measure knowledge/skills, self-efficacy, and practices regarding weight management at baseline and three-month post-intervention. Results: Overall, the knowledge/skills, self-efficacy, and practices related to obesity management among GPs were improved. There were significant increases in the frequencies of all items describing weight management practice after the intervention (P<0.05). The number of participants who rated themselves at the “high” level of weight management skills/knowledge increased significantly (P<0.05). The scores of self-efficacy increased in eight items, with the total score of the scale were observed to be increased when compared to pre-intervention (P<0.05). Conclusion: The integrated intervention program improved GPs’ knowledge/skills, self-efficacy, and professional practices. Comprehensive and specific strategies based on GPs’ professional behaviors and attitudes are expected to be developed in the future.
Keywords: Weight management; Intervention; Community health; Overweight; Obesity
What is known about the topic?
General Practitioners (GPs) play a major role in weight monitor and management of patients by facilitating behavior changes.
Health care professionals do not routinely provide assessment and intervention for their patients with recommended strategies.
Little is known about the self-efficacy of GPs and its effect on the practice of weight management among adult patients.
What does this paper add?
Overall, GPs’ knowledge/skills, self-efficacy and practices in weight management in China were unsatisfactory.
A combined training program significantly improved GPs’ knowledge/skills, self-efficacy, and practice in weight management.
Future interventions may also target the relatively low knowledge and skills among GPs.
Obesity was once considered a problem only for high-income countries. However, in recent years, developing countries are also experiencing an increased prevalence of obesity. The 2014 China National Physique Monitoring Bulletin of a large random sample (n=531,849) reported an elevated prevalence of both overweight (32.7%) and obesity (10.5%) [1].
In response to the rapidly growing prevalence of obesity, the Chinese Guidelines for Prevention and Control of Overweight and Obesity in Adults [2] recommend that primary care clinicians, especially General Practitioners (GPs), are responsible for monitoring and managing patients’ weight by assisting in behavior changes. In 2016, there were approximately 209,000 GPs in China [3]. These individuals are responsible for health consultation, epidemic prevention, community rehabilitation, chronic disease management, and other health services in the primary healthcare system. However, GPs do not routinely provide assessment and intervention for their patients with recommended strategies. An earlier study found that only 55% GPs assessed patients’ weight and 25% evaluated daily exercise in the US. [4]. Yet, after over 20 years, the practice of weight management remains unsatisfactory. A nationally representative survey conducted in 2008 found that only half (49%) GPs recorded Body Mass Index (BMI) regularly and less than 50% provided specific guidance on diet, physical activity, and/ or weight control [5]. A longitudinal study found no change in the positive response to the statement “Noticing patients overweight and guidance of treatment” in GPs over the course of 15 years (1992-2007). Additionally, GPs rarely provided advice on nutrition during daily practice and their self-efficacy regarding overweight management has declined [6]. Although GPs typically think weight management is important, their self-efficacy in weight management is low [7]. A Chinese survey of 904 medical personnel in primary care units found that only 23.6% GPs calculated patients’ BMI, 16.2% measured waistline in their daily practice, and 26-30% provided instructions on specific diet, exercise guidance, and/or emotional support [8].
Given the high prevalence of obesity and unsatisfactory practice of weight management by GPs in China, it is necessary to increase GPs’ awareness of the importance of their role in weight management. Mastering the knowledge and skills for weight management may be the first important step to solve the ubiquitous long-standing problems with GPs in the worldwide. Therefore, well-designed interventional studies targeting essential components are needed.
Previous studies reported factors influencing professional practices of healthcare providers, such as relevant knowledge, training, and selfefficacy [9]. Social Cognitive Theory (SCT) proposes that an individual’s self-efficacy in their ability to successfully change behavior is an essential factor in behavior change [10]. Self-efficacy was found a key predictor directly and positively influencing weight management practices by our previous studies and other quantitative researches [8,11]. Health care clinicians with higher self-efficacy about weight management were more likely to start or maintain an intervention implementation even in the face of existing barriers [12]. A study of pediatricians conducted in 2005-2006 found that interventions targeting self-efficacy significantly improved weight management practice [13]. Similarly, several qualitative studies reported that low self-efficacy is a major barrier to the use of guidelines for the management of obesity by GPs [6,14,15].
So far, few interventional studies have focused on the self-efficacy of GPs and its effect on the practice of weight management among adult patients. Therefore, the aim of this study was to evaluate the effect of an integrated intervention program targeting self-efficacy on GPs’ clinical practice of weight management. Findings from this study will provide evidence on possible solutions to the existing difficult problems about health and nutrition with GPs.
Design
A quasi-experimental (pre-test and post-test) design was used.
Participants
A convenience sample of 118 GPs was recruited from two community health service centers in the Pudong New Area of Shanghai, China. GPs with at least one year of work experience were included in the study. Exclusion criteria included: (1) medical staff engaged in child health care or (2) unwilling to participate in the study.
The study was approved by the ethics committee of the Institutional Review Board of Second Military Medical University in Shanghai, China and informed consent were obtained from each participant in the first page of the questionnaire. No subjects received compensation for participation in the current study.
Interventions
An integrated intervention program, including training lectures and educational materials, was developed to promote the professional practice of GPs about obesity and overweight management.
These interventions aimed to increase GPs’ knowledge/skills and to provide environment/resources for the GPs, which were related to self-efficacy. Knowledge/skills have been reported a key factor in the initiation of professional behavior change [14,16-18]. Environment/ resources included assessment tools, weight management guidance, and other educational materials. The absence of these elements has been a barrier to primary health professionals performing weight management [14,15,19]. According to the Theory of Planned Behavior, knowledge (among other variables) can indirectly cause behavior change by influencing self-efficacy, suggesting that self-efficacy works as a mediator in the context of work performance. A causal relationship between knowledge and self-efficacy has been reported [20-22]. Our earlier work showed that both variables (e.g., knowledge/skills and environment/resources) positively influenced self-efficacy and weight management practice of GPs. Collectively, training, availability of educational materials, and auxiliary tools can improve the self-efficacy of primary health professionals [23-25]. Therefore, this study provided training lectures and educational materials as interventions to promote self-efficacy and practice by improving GPs’ knowledge/skills and providing environment/resources.
Training lectures: Two 100 min training sessions were co-hosted by two community health service centers. The content of the training was designed according to recommended weight management practice from the Chinese Guidelines for Prevention and Control of Overweight and Obesity in Adults. The first training session was held in July 2016. It included a review of overweight and obesity in adults; the role of primary medical staff in weight management; an introduction to obesity diagnosis, control, and treatment in primary care units; and general knowledge/skills related to counseling. The second training session was held two weeks later. It focused mainly on nutrition and dietary interventions on overweight and obesity, upon the request of the majority of the GPs. This training session included information, such as screening patients, calculating appropriate caloric intake, and developing a reasonable diet for patients with obesity.
Educational materials
Educational materials included:
(1) Implementation guideline: The Chinese Guidelines for Prevention and Control of Overweight and Obesity in Adults was provided to every participant. The guidelines made it possible for participants to learn more about the standard practices of weight management and refer to it for more details as needed.
(2) Assessment tool: A measuring tape was designed with two rotatable concentric dials (weight and height) to determine the BMI of patients in seconds. The GPs were recommended to use this tool to measure the waist circumference, evaluate the body type, and provide weight-loss advice for those patients requiring it.
(3) Patient brochure: A culturally appropriate weight management brochure, including the epidemic trend, risks, stages, complications, and control of obesity, was designed for patients to read and use in self-monitoring. In this document, there was also a chart for doctors to record the date and weight to observe dynamic weight change. The brochures were available in every consulting room.
(4) Educational poster: Posters were designed to show the prevalence, risk, prevention, and self-management of weight. The posters were informal, patient-centered, culturally appropriate, and at a suitable literacy level. They were kept in prominent locations for more than three months, such as at registration and on the bulletin board in both community health service centers. Patients could learn from the posters and request further information from doctors when necessary. In addition, the strong atmosphere helped to improve GPs’ awareness of weight management as well as participate in the promotion of obesity management. The posters were also used as a strategy to recruit participants.
Procedures: Data were collected at two time points (baseline and after the three-month intervention). After the collection of the baseline survey in June 2016, educational materials were provided. Afterward, two 100 min training sessions were held within the following month. We encouraged all eligible GPs to attend the training section and provided them with educational materials at the same time.
Data were collected via three self-reported scales in September 2016, which have been previously determined as reliable and valid [26]. The researcher distributed the questionnaires to participants at the two community health centers and collected the questionnaires immediately upon completion. In the case of multiple or missing answers, the participant was asked to clarity. It took approximately 12 min to complete the survey.
Variables of interest
Weight management practices: Weight management practices were assessed using an 8 item self-rating scale, which evaluated the percentage of patients who received each practice of weight management from the participant during the previous month [26]. The items included professional practices related to the recommended guidelines, such as weight assessment, patient counseling, and emotional support [2]. The response to every item was scored from 1 (0-25%) to 4 (75-100%). Choosing 1 (0-25%) was considered as lowlevel practice in weight management while choosing 3 (50-75%) and/or 4 (75-100%) was considered as high-level practice. The Cronbach’s α of this subscale was 0.95. The numbers of individuals indicating high-level and low-level practice were compared before and after the intervention program, respectively.
Knowledge/skills regarding overweight and obesity management: Knowledge/skills of weight management were assessed using a 9 item self-rating scale, which was developed to evaluate GPs’ theoretical or practical understanding and competence to perform weight management practices. The 9 items represented one domain with 58.18% variance in the exploratory factor analysis. Participants evaluated their own knowledge/skills and chose the best option from 1 (Low level) to 3 (High level). The Cronbach’s α of this subscale was 0.91. The number of participants with a high-level and low-level of knowledge/skills was compared with those before the intervention program, respectively.
Self-efficacy for weight management practices: Self-efficacy [27], defined as a persons’ belief in his/her capability to perform a specific task or achieve a certain result, is a key driver of professional practice implementation within the healthcare setting. A 9-item scale was used to evaluate the self-efficacy for weight management of participant, with each item scored from 1 (Not at all confident) to 6 (Totally confident). The total score ranges from 9 to 54. The Cronbach’s α of this scale was 0.94.
Statistical analysis
The primary outcome was the change in the scores of weight management practice, knowledge/skills, and self-efficacy. Descriptive statistics were used, including mean and standard deviation for continuous variables, and percentage for categorical variables. Student’s t-test and Chi-square test were used to examine the differences between groups for continuous variables and categorical variables, respectively. The analyses were performed using SPSS software (version 18.0, IBM, New York, US). The difference was considered statistically significant at α=0.05.
Characteristics
From the two community health service centers, 118 individuals met the inclusion criteria. There was a difference in the number of preand post-intervention questionnaires due to the voluntary nature of participation. The baseline and post-intervention characteristics were compared to confirm the consistency of demographic and professional characteristics (Table 1). No significant differences were observed between the two time points.
| Characteristics | Pre-Test n (%)or `x (SD)a |
Post-Test n (%)or `x (SD)a |
t or χ2b | P |
|---|---|---|---|---|
| Age | 37.07 (7.04) | 37.05 (6.95) | 0.018 | 0.986 |
| Working years | 14.63 (9.96) | 14.53 (8.08) | 0.087 | 0.931 |
| Gender | 0.003 | 1.000 | ||
| Female | 82 (69.5) | 81 (69.8) | ||
| Male | 36 (30.5) | 35 (30.2) | ||
| Job titles | 0.029 | 0.985 | ||
| Primary | 44 (37.3) | 42 (36.2) | ||
| Intermediate | 68 (57.6) | 68 (58.6) | ||
| Senior | 6 (5.1) | 6 (5.2) | ||
| Educational levels | 0.004 | 0.998 | ||
| Associate degree or below | 7 (5.9) | 7 (6.0) | ||
| Bachelor’s degree | 97 (82.2) | 95 (81.9) | ||
| Master’s degree or above | 14 (11.9) | 14 (12.1) |
a. Results were described in the form of 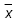 (SD) for continuous variables and n (%) for categorical variables.
(SD) for continuous variables and n (%) for categorical variables.
b. Student’s t-test was used to explore differences between pre-test and post-test for continuous variables, and χ2 test for categorical variables.
Table 1: Characteristics of pre-prevention (n=118) and post-prevention (n=116) participants.
Changes in professional practices
We considered implementing weight management for more than 50% patients in a month as a high-level of practice and calculated the number of GPs who reported this level. Data are presented in Table 2. There were significant improvements in the weight management practice after the intervention (P<0.05). To explore whether there was improvement among participants who performed weight management in less than 25% patients before the intervention, we compared the number of participants who chose 1 (<25%) before and after the intervention. The results suggested that the percentage of GPs who rarely performed weight management significantly decreased after the intervention program (P<0.05).
| Behavior about weight management | High level n (%)a |
P | Low level n (%)b |
P | ||
|---|---|---|---|---|---|---|
| Pre-Test | Post-Test | Pre-Test | Post-Test | |||
| 1. BMI assessment. | 35 (29.7) | 44 (37.9) | 0.214 | 63 (53.4) | 34 (29.3) | < 0.001 |
| 2. Waist circumference measurement. | 25 (21.2) | 31 (26.7) | 0.360 | 71 (60.2) | 45 (38.8) | 0.001 |
| 3. Further assessment and physical examination. | 39 (33.1) | 42 (36.2) | 0.681 | 62 (52.5) | 30 (25.9) | < 0.001 |
| 4. General lifestyle advice about weight management. | 47 (39.8) | 63 (54.3) | 0.036 | 50 (42.4) | 22 (19.0) | < 0.001 |
| 5. Detailed/tailored advice about diets (e.g., restricted calorie diets). | 33 (28.0) | 52 (44.8) | 0.010 | 54 (45.8) | 31 (26.7) | 0.003 |
| 6. Detailed/tailored advice about physical activity (e.g., frequency,duration, and intensity of exercise). | 34 (28.8) | 49 (42.2) | 0.040 | 55 (46.6) | 28 (24.1) | < 0.001 |
| 7. Information resources about weight control. | 30 (25.4) | 44 (37.9) | 0.049 | 62 (52.5) | 31 (26.7) | < 0.001 |
| 8. Emotional support. | 26 (20.0) | 48 (41.4) | 0.002 | 64 (54.2) | 30 (25.9) | < 0.001 |
| a.High level n (%): Each item was described by the number (percentage) of participants who chose 3 (50–75%) and 4 (75–100%). b. Low level n (%): Each item was described by the number (percentage) of participants who chose 1 (<25%). |
||||||
Table 2: Weight management practice before and after the intervention program.
Changes in knowledge/skills
Overall, PGs’ knowledge/skills improved after the intervention (Table 3). The number of participants who rated themselves at a high level increased significantly in six of the nine items (P<0.05). The number of participants who rated themselves at a low level decreased significantly in seven of the nine items (P<0.05).
| Knowledge/skills of weight management | High level n (%) a |
P | Low level n (%) b |
P | ||
|---|---|---|---|---|---|---|
| Pre-Test | Post-Test | Pre-Test | Post-Test | |||
| 1. The meaning and calculation of BMI | 65 (55.1) | 72 (62.1) | 0.291 | 14 (11.9) | 4 (3.4) | 0.025 |
| 2. Calculation of waist and hip circumference | 57 (48.3) | 74 (63.8) | 0.018 | 16 (13.6) | 7 (6.0) | 0.077 |
| 3. Assessment of degree of overweight | 61 (51.7) | 66 (56.9) | 0.434 | 15 (12.7) | 4 (3.4) | 0.015 |
| 4. Harm of overweight and obesity | 66 (55.9) | 79 (68.1) | 0.060 | 8 (6.8) | 4 (3.4) | 0.375 |
| 5. Guidance on self-monitor | 40 (33.9) | 57 (49.1) | 0.024 | 21 (17.8) | 8 (6.9) | 0.016 |
| 6. Setting a weight-loss goal and making a tailored plan | 21 (17.8) | 44 (37.9) | 0.001 | 39 (33.1) | 16 (13.8) | 0.001 |
| 7. Guidance on modification of eating practices | 20 (16.9) | 45 (38.8) | < 0.001 | 47 (39.8) | 17 (14.7) | < 0.001 |
| 8. Guidance on modification of physical activity | 24 (20.3) | 42 (36.2) | 0.008 | 32 (27.1) | 11 (9.5) | < 0.001 |
| 9. Considerations for drug treatment (e.g., dosage, side effect). | 23 (19.5) | 39 (33.6) | 0.018 | 56 (47.5) | 22 (19.0) | < 0.001 |
a. High level n (%): Each item was described by the number (percentage) of participants who chose 3 (high level)
b. Low leveln(%): Each item was described by the number (percentage) of participants who chose 1 (low level)
Table 3: Knowledge/skills before and after the intervention program.
Self-efficacy change
The intervention improved PGs’ self-efficacy. The scores increased significantly in eight of the nine questions (P<0.05). Additionally, the total score improved significantly after the intervention program (P<0.001). Data are presented in Table 4.
| Item | Item score: x (SD)a | P | |
|---|---|---|---|
| Pre-Test | Post-Test | ||
| • I believe I can perform a BMI assessment. | 3.55 (1.34) | 4.16 (0.96) | <0.001 |
| • I believe I can perform a waist circumference measurement. | 3.45 (1.24) | 4.10 (0.97) | <0.001 |
| • I believe I can help patients prevent his/her weight from getting higher. | 3.38 (1.37) | 3.98 (1.17) | <0.001 |
| • I believe I can help patients lose weight. | 3.49 (1.30) | 3.97 (1.16) | 0.003 |
| • I believe I can provide general advice about weight control(e.g., monitor waist circumference, calculate BMI). | 4.42 (1.37) | 4.58 (1.00) | 0.301 |
| • I believe I can provide detailed/tailored advice about diets (e.g., restricted calorie diets). | 3.83 (1.40) | 4.28 (1.03) | 0.006 |
| • I believe I can provide detailed/tailored advice about physical activity(e.g., frequency,duration, and intensity of exercise). | 3.76 (1.41) | 4.32 (1.03) | 0.001 |
| I believe I can provide information resources about weight control. | 3.97 (1.32) | 4.28 (1.05) | 0.049 |
| • I believe I can provide emotional support for patients. | 3.95 (1.31) | 4.47 (1.02) | 0.001 |
| Total score | 33.81 (10.17) | 38.17 (7.93) | <0.001 |
a.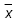 (SD): Each item score and the total score was described by the mean (standard deviation).
(SD): Each item score and the total score was described by the mean (standard deviation).
Table 4: Self-efficacy before and after the intervention program.
In this study, an integrated intervention program based on the SCT was administered to GPs in Shanghai. This intervention, composed of training lectures and educational materials, was found to be effective in improving the knowledge/skills, self-efficacy, and practices of GPs regarding overweight and obesity management.
Previous studies have reported that the knowledge and self-efficacy of healthcare providers in patient counseling improved significantly after training [28]. Similarly, our interventions were effective in improving GPs’ knowledge/skills regarding weight management. We found that the number of participants with high-level knowledge/skills increased significantly in six of the nine items after the intervention. The other three items with no significant changes describe the basic knowledge/ skills related to weight management, including BMI calculation, weight assessment, and understanding of the harm caused by obesity. Before the intervention, scores of these three items were significantly higher than the others (over 50% GPs chose high level). This finding suggests a possible ceiling effect and that other forms of training may be more effective than lectures in promoting GPs’ knowledge/skills evaluated by these specific items. The percentages of participants with a high-level in these items were not significantly improved. However, when comparing the number of participants who chose 1 (low level) after intervention with those who chose 1 before the intervention, we found two of these three items experienced a decrease in GPs with low-level knowledge/ skills, which also showed a positive effect of the intervention program on the improvement of these items. Collectively, these results suggest that the design of interventions met the study objective, and that future intervention should also target the relatively low-level knowledge/skills reported by the participants.
We chose two community healthcare service centers in Shanghai, the most developed city in China. The relatively high education level and a large amount of continuing training may have equipped the study participants with more basic knowledge/skills, such as measurement, assessment, pathogenesis, and general advice about overweight and obesity. However, despite the substantial general knowledge/skills, a severe lack of some specific knowledge/skills was noted, such as setting an individual weight-loss goal or plan according to BMI and health status. This finding suggests a higher educational need for specific knowledge/skills, rather than general knowledge/skills, related to weight management. Therefore, future research should focus on training programs/educational materials that provide details about the tactics for setting a goal, planning, and intervening regarding diet and/ or exercise according to the severity of obesity, physical condition, and/ or co-morbidities of the patient.
Self-efficacy has been considered one of the most important factors influencing professional practices of health care clinicians in many studies [29,30]. In our research, self-efficacy was evaluated using a self-designed questionnaire, which was well-researched and had adequate validity and reliability. After the interventions, most items scored significantly higher, which suggested positive effects of the intervention. This finding is consistent with a previous randomized controlled trial, which showed the positive effects of training on diet and physical activity on pediatric nurses’ self-efficacy in preventing childhood obesity [31].
In this study, weight management practices included assessment, counseling, intervention, and support for overweight and obesity. The questionnaire had eight items that evaluate the frequency of implementation during the past month. The results showed significant improvement of high-level practice in five items after the intervention and a significant decrease of low-level practice in all items. The trained participants with more knowledge and skills may have a higher level of self-efficacy in weight management. The training may also have encouraged the participants to perform weight management because of the rich environment created by the posters. Furthermore, educational materials not only provided more information about weight-loss but also made the assessment and intervention more convenient, which is consistent with other studies [32-36]. A pilot study conducted in a public hospital showed that training and materials focused on weight management significantly improved physician counseling and patients’ recall of weight loss recommendations from their doctors [37].
We found that knowledge/skills improved substantially after the intervention, parallel with the increase of self-efficacy results. This study showed that knowledge/skills and self-efficacy, rather than corresponding practices, increased to a relatively high level. It was noted that the score of each item describing practices remained low after the intervention. For instance, the highest score for the item, “Give general lifestyle advice about weight management,” was provided by only 54.3% the GPs after the intervention. This finding suggests other unmeasured variables may have directly or indirectly affected practices, such as material resources, organizational climate, and/or social support [14,16,37]. In addition, psychological factors may play an important role. Obesity is a sensitive topic for some people. These individuals often feel ashamed or guilty when confronted by others about their obesity. Therefore, GPs may be hesitant to discuss obesity, especially when their patients do not have serious acute complications related to overweight/ obesity, as discussing it may impair the GP-patient relationship.
In this study, we examined a novel intervention strategy among GPs in China. Nonetheless, this study has several limitations. First, blinding was difficult to achieve because the survey was performed by a self-rating questionnaire. As such, when the participants completed the second survey following the training, they were aware of what was being observed. They may change their responses due to intention to please and social expectation. Future research could address this issue by also surveying patients following examination to determine if the percentages align with the recollection of GPs. Furthermore, the convenience sampling method and the small sample limited the generalizability of the study findings. Future studies should address these limitations to enhance the casualty inference. Finally, we selected a 3 month follow-up period, which may be short. In the future, other time points should be examined to explore whether there is a difference between the immediate and continued effect after the intervention.
Obesity is a common problem across the world. However, health care professionals do not routinely perform weight management with recommended strategies. In response to the challenges with GPs in the sectors of Health and Nutrition, we conducted a pilot study to evaluate whether an integrated intervention program based on the self-efficacy theory could promote GPs’ weight management practice in China. The combined training and educational material intervention were effective in improving healthcare professionals’ knowledge/skills, self-efficacy, and practice. Further research is needed to confirm our findings in a more representative and larger sample. A longer follow-up period is warranted to detect the long-term effects of the intervention. Comprehensive and specific strategies based on GPs’ professional behaviors and attitudes are urgently needed.
The authors would like to thank Jinyang and Hudong community health care services and the time taken by participants completing the survey and receiving interventions.
The authors appreciate financial support from National Natural Science Foundation of China (71303250), Shanghai Natural Science Foundation (13ZR1449200) and Shanghai Municipal Education Commission-Nursing Gaoyuan Project (Hlgy1601dxk).
The authors declare no conflict of interest.