Review Article - (2019) Volume 1, Issue 1
Introduction: Van der Woude Syndrome (VWS) consists of a genetic abnormality attributed to mutations in the IRF6 gene, characterized by the presence of paramedian pits in the lower lip, cleft lip and/or palate and hypodontia. Phenotypes of the syndrome are related to the oral cavity, and then other dental anomalies would also be present in this specific syndrome.
Objective: The aim of this study was to identify different dental phenotypes in subjects with VWS through an integrative review of the literature.
Materials and methods: A systematic search was conducted in Pubmed/Medline for articles which assessed dental phenotypes in van der Woude syndrome.
Results: Six publications were selected, considering the eligibility criteria of the articles. Different dental phenotypes are described in this syndrome. Tooth agenesis is the most common phenotype and is already associated as one of the characteristics of the syndrome. However, taurodontism has also been reported with a prevalence of 46% in these patients.
Conclusion: It is important to understand the nature and extent of the dental phenotype variation in VWS patients, allowing an adequate approach to oral rehabilitation planning for these patients.
Tooth abnormalities, Van der Woude syndrome, Cleft lip, Cleft palate, Taurodontism.
Van der Woude syndrome is a genetic abnormality with an inherited pattern characterized as autosomal dominant, with variable expression. Initially, the congenital pits on the lower lip were described by Demarquay in 1845. Anne van der Woude reported the syndrome for the first time in 1954, considering the presence of the congenital pits in the lower lip associated with cleft lip and palate, which occurred in 80% of cases. Van der Woude also confirmed that the cases had a hereditary character and to characterize and diagnose the syndrome, the fistulas in the lower lip and the cleft lip and/or palate were considered as the main phenotypes [1]. According to Burdick [2] the occurrence of this syndrome ranges from 1: 100,000 to 1: 40,000 live births.
Regarding the etiology, Ingraham et al. [3] affirmed the correlation between mutations in the IRF6 gene and the Van der Woude Syndrome. The IRF6 gene (Interferon Regulatory Factor 6) belongs to a family of transcription factors. The variants in the IRF6 are known to be associated with syndromic FL (P) and also contribute to the risk of isolated or non-syndromic FL with or without FP. Approximately 70% of cases of VWS are attributed to the mutations distributed in the IRF6 gene [2].
According to Schutte et al. [4], patients with VWS may present congenital (usually bilateral) pits in the lower lip, cleft lip and/or cleft palate, and may present only one or several of these signs. However, its most striking feature is the presence of congenital pits in the lower lip, which may be the only manifestation of the syndrome [5].
In relation to phenotype the cleft lip and/or palate, the VWS represents the most common syndromic form of this phenotype, affecting about 2% of all patients with clefts [5,6].
In addition to classical phenotypes, these individuals may also present other intraoral abnormalities such as hypodontia, hypoplasia, dental malformations, and supernumerary teeth that should be diagnosed and treated at an early stage for functional and aesthetic rehabilitation [7]. Other oral manifestations also mentioned include ankyloglossia and high arched palate [5,7].
The most common dental phenotype associated with VWS is hypodontia. According to Ranta and Rintala [8] the high frequency of hypodontia in their studies shows that tooth agenesis can be considered an important characteristic in the diagnosis of Van der Woude syndrome. The study conducted by this group of researchers showed a considerable difference between the prevalence of tooth agenesis in subjects with VWS (69%) when compared to non-syndromic individuals in the control group (43%).
However, because the main features of the syndrome are related to the oral cavity, it would be expected that other dental phenotypes, besides tooth agenesis, could be present in this specific syndrome. However, studies investigating or even describing other dental phenotypes diagnosed in subjects with Van der Woude syndrome are scarce.
Considering that it is important to understand the nature and extent of dental phenotype variation in VWS individuals, and are thus able to perform a better diagnosis and appropriate therapeutic behavior in each particular case, the present study proposed an integrative literature review in order to describe the different dental phenotypes in individuals with Van der Woude syndrome, addressing aspects related to the frequency of occurrence of these dental anomalies in the context of the syndrome.
The present study used as a research strategy a systematic search in PubMed and Medline databases published in the last fifteen years, using the descriptors “VAN DER WOUDE SYNDROME” and “TOOTH ABNORMALITIES”, by the combination (Van der Woude syndrome and tooth abnormalities) in the search of keywords in databases.
The studies collected in the databases entered into a cautious process of selection, where criteria of eligibility of the found articles were established in order to keep the focus of the study on the main theme.
The titles and abstracts were examined and judged by two independent examiners according to the following inclusion criteria: only articles of the last fifteen years, indexed in the PubMed/Medline databases, written in English and related to dental anomalies in Van der Woude syndrome. All studies outside the main theme, studies in languages other than English, and published more than fifteen years ago were excluded from the present review.
The data collection process consisted of the search for keywords with the combination (Van der Woude syndrome and tooth abnormalities) in PubMed/Medline in the last fifteen years generated seventeen results, and in the Medline database were the same studies as Pubmed. However, the PubMed database featured additional studies with these keywords. Of the seventeen papers resulting from the search, five were excluded because they focused on genetics, two were not available in English (Italian and Chinese) and four did not address the main theme of this review, which is the description of dental phenotypes specifically in the Van der Woude Syndrome. Thus, six studies were selected for the present study. There was consensus between the two examiners regarding the studies selected to compose the present review. All data concerning the dental phenotypes diagnosed in subjects with the Van der Woude syndrome were extracted from the papers.
The six papers selected for this literature review were three clinical trials and three clinical cases, as presented in Figure 1. Regarding the geographical location where the studies were conducted, the clinical cases were from India, Italy and China and the clinical investigations were two from the United States and one from Australia.
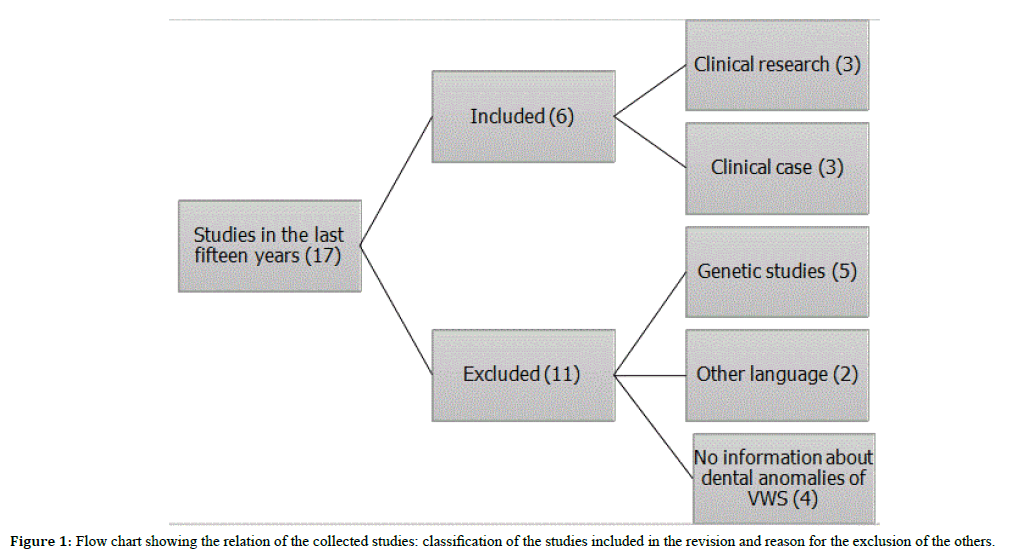
Figure 1. Flow chart showing the relation of the collected studies: classification of the studies included in the revision and reason for the exclusion of the others.
All phenotypes described in the reviewed papers are presented in Table 1. In the clinical case reports, three different types of dental phenotypes were found in subjects with the Van der Woude syndrome: agenesis (most common anomaly found in all cases), fusion and dental transposition. The method used in these studies to diagnose the different phenotypes was clinical examination and radiographic analysis, except for Bardazzi et al. [9], who used only the clinical examination. In all the clinical cases reported, the subjects were male, with ages varying between seven and thirtytwo years and had paramedian pits in the lower lip, a characteristic that is very important for the diagnosis of the syndrome. As to the presence of the cleft and the type, these studies were: two patients with bilateral cleft lip and palate, one with cleft palate only and one patient who did not present cleft.
| Author | Year | Country and population | Type of study | No. of subjects | Gender (n) | Age (n) | Dental phenotype | Teeth most affected | Type of cleft | Other findings |
|---|---|---|---|---|---|---|---|---|---|---|
| Sarode et al. [21] | 2011 | India | Clinical case | 1 | M (1) | 7 (1) | Fusion | 72 and 73 | BCLP | Pits Ankyloglossia |
| Agenesis | 52,62,12.22 | |||||||||
| Lam et al. [16] | 2010 | Australia | Clinical research | 22 | M (10) | -- | Agenesis (86%) | upper lateral incisors and 2ºPM (6) (27%) | BCLP (32%) UCLP (32%) SCP (23%) CP (9%) | Pits Persistence of the ductus arteriosus |
| F (12) | Molar Incisor Hypomineralization (4.5%) | -- | ||||||||
| Nawa et al. [10] | 2008 | United States | Clinical research | 13 | M (8) | 9 (3) | Taurodontism (46%) | U-T (3) (50%) | BCLP (4) (31%) UCLP (2) (15%) | -- |
| F (5) | 10 (4) | B-T (3)(50%) | ||||||||
| 11 (3) | Agenesis (77%) | 15, 12, 22, 25, 35, 45, 32, 11, 21. | SCP (2) (8%) CP (5) (38%) | |||||||
| 12(1) | ||||||||||
| 13 (2) | ||||||||||
| Bardazzi et al. [9] | 2006 | Italy | Clinical case | 1 | M (1) | 32 (1) | Agenesis | 11, 13, 14, 15 | None | Pits |
| Oberoi and Vargevik [17] | 2005 | United States | Clinical research | 15 | M (9) F (6) | 5 a 13 | Agenesis (73%) | 35 and 45 | BCLP (4) (27%) UCLP (3) (20%) CP (6) (40%) SCP (2) (13%) | Maxillary hypoplasia |
| King et al. [22] | 2004 | China | Clinical case 1 | 1 | M (1) | 19 (1) | Agenesis | 12, 35 and 45 | CP | Pits |
| Transposition | 13 and 14 | |||||||||
| Clinical case 2 | 1 | M (1) | 13 (1) | Agenesis | 52,62,12,22, One (1) lower incisor (deciduous and permanent) | BCLP |
Table 1: Data on the dental phenotypes obtained from the selected articles.
Regarding the clinical research, there was an equivalent distribution between the sexes and the predominant age group was between five and thirteen years. In these three clinical studies, three different types of dental phenotypes were described: tooth agenesis (most prevalent anomaly), taurodontism and molar incisor hypomineralization. The diagnostic method used to evaluate the different dental phenotypes was variable in these studies.
All researches found a high occurrence of tooth agenesis, ranging from 73% to 86% of the subjects presenting this phenotype as part of the clinical picture of the syndrome. The teeth groups most affected by agenesis were the second premolars. Taurodontism was investigated only in the research of Nawa et al. [10] and these authors found a prevalence of 46% for this phenotype.
In the bibliographic survey, seventeen papers published in the period from 2003 to 2018 were initially selected. However, the focus on dental phenotypes is still limited, since only six clearly addressed the diagnosis of these characteristics. Therefore, the main clinical focus of the publications related to the Van der Woude syndrome are paramedian pits in the lower lip followed by the presence of cleft and few publications investigate dental phenotypes. In addition to the clinical features, many studies have been conducted investigating the genetic aspect of the syndrome. Authors such as Khandewal et al. [11], Vieira et al. [12], Pegelow et al. [13], Ye XQ et al. [14] and Item et al. [15] have publications with specific focus on molecular investigation, most of them describing the different mutations in the IRF6 gene found in subjects with the syndrome.
In the present integrative literature review, only those papers that presented or described the different types of dental phenotypes in the Van der Woude syndrome were used, leading to the exclusion of a significant number of studies that did not present specific data in this main focus.
In spite of presenting distinct objectives, the six papers selected for the present review have in common the description of numerous dental phenotypes found in subjects with the syndrome. Although each study focused on the investigation of one or two specific dental alterations, when analyzing all the studies, it was possible to verify that the most common anomalies found in the VWS were tooth agenesis and taurodontism.
Hypodontia is already considered a classical phenotype within the clinical feature of the Van der Woude syndrome [8]. The occurrence of hypodontia in patients with cleft has been attributed to multiple factors, such as genetic and environmental factors, altered mesenchymal differentiation and direct effect of cleft in odontogenesis. Tooth agenesis may contribute to atresia of the arches, especially the maxilla, and this may result in dental malocclusion and skeletal discrepancies between the arches, which may require orthodontic and/or orthopedic intervention [16]. It is extremely important that the dentist is aware of these implications in the oral cavity in order to achieve a better treatment plan for the child.
Lam et al. [16] in a clinical study evaluated, by clinical and radiographic examination, a sample of twenty-two individuals with VWS with no reported age and revealed a prevalence of 86% of agenesis. The teeth most affected by this phenotype were the upper lateral incisors, followed by the second premolars. The authors also pointed out that the different types of clefts (UCLP, BCLP, CP and SCP) were associated with agenesis of at least one tooth. A single subject of this sample presented molar incisor hypomineralization, an anomaly that is probably not related to the syndrome in question, but to other factors of dental development, since it occurred in an isolated case and there are in the literature reports of this type of dental phenotype associated with the VWS.
Oberoi and Vargevik [17] conducted a retrospective clinical study investigating the prevalence of tooth agenesis by means of medical records and radiographs using a sample of fifteen individuals with VWS aged five to thirteen years. The authors found a prevalence of agenesis of 73%. In their studies, they showed a higher prevalence of this phenotype in the lower second premolars, with no predominance of one side in VWS patients, whereas in the control group of patients with cleft lip and palate without the syndrome, there was a predominance of second premolar agenesis on the left side.
Nawa et al. [10] also carried out a retrospective study using charts and radiographs of thirteen individuals with VWS ranging in age from nine years and two months to thirteen years and eleven months. The authors found a prevalence of 77% of tooth agenesis in subjects with VWS, and the most affected teeth were the upper lateral incisors and the second lower premolars. In addition to this anomaly, using the method of Seow and Lai [18] that uses as a reference the measurement of the lower first molars for teeth classification with hypo, meso or hyperaurodontism, the authors found 46% of the individuals in their sample with a diagnosis of taurodontism, an anomaly which until then had not been associated with the VWS, but which was previously associated with Down syndrome [19] and with the non-syndromic Pierre Robin sequence [20]. This high frequency of hypodontia and taurodontism in subjects with VWS may have a common etiology, leading to the hypothesis that the syndrome and these two anomalies could present a similar genetic mechanism that would lead to their occurrence. Taurodontism also represents a relevant phenotype, since it may increase the risk of pulpal exposure during restorative procedures, as well as the potential risk of root resorption during orthodontic treatment since the roots may present very small dimensions. Therefore, it is indispensable that the dental surgeon be aware of the possibility of occurrences of this dental phenotype in VWS subjects.
Dental fusion was described in the study by Sarode et al. [21] in which they reported a case of a 7-year-old male with VWS. In addition to the tooth agenesis of the deciduous and permanent maxillary lateral incisors, there was also fusion of the teeth 72 and 73, an unusual anomaly in syndrome and not necessarily directly related to VWS, probably a chance occurrence, since in the literature there is no correlation of this anomaly with the syndrome.
The other two cases described by Bardazzi et al. [9] and King et al. [22] presented cases of subjects with tooth agenesis of numerous dental elements. In the study by King and colleagues, the researchers also diagnosed dental transposition of teeth 13 and 14 as an additional phenotype, but also possibly not directly related to VWS.
In the study by Bardazzi et al. [9], the authors used only the clinical examination as a diagnostic method for hypodontia. Taking into consideration the subject's age (32 years), it is possible to infer that there may be other factors that led to the loss of teeth 11, 13, 14 and 15, other than hypodontia.
King et al. [22] reported two clinical cases with male subjects through clinical examination and radiographic analysis. In case 1, the 19-year-old man presented agenesis of teeth 12, 35 and 45 and cleft palate. In the second case, a 13-year-old man presented agenesis of the deciduous and permanent upper lateral incisors, as well as the agenesis of a lower incisor (deciduous and permanent) and a bilateral cleft of the lip and palate.
In the general context of the analysis of the studies, it is possible to infer that the most common dental phenotype in the VWS is tooth agenesis, especially affecting the upper lateral incisor teeth and second premolars, which were already expected, since agenesis is already considered a feature of this syndrome according to the literature. However, the data on the prevalence of taurodontism, around 46%, draws attention and leads us to reflect if this could not be new dental phenotype to be considered, in addition to the possibility of the association of the two phenotypes, agenesis and taurodontism in this syndrome. Further confirmation of this hypothesis would require additional research investigating this phenotype in the VWS context.
We would like to thank the Brazilian Ministry of Health for the support.
Aline Cristina da Silva Trevizan (ACST), Pollyana Pereira Teotonio dos Santos (PPTS), Maria Carolina de Moraes Pereira (MCMP), Lucimara Teixeira das Neves (LTN)
Author ACST participated in the design, execution and analysis of the paper. Author PPTS participated by selecting articles for review. Author MCMP participated by selecting articles for review and co-wrote the paper. Author LTN conceived the original idea, analysis of the paper and supervised the review. All authors discussed the results and contributed to the final manuscript.
Received: 14-Aug-2019 Published: 30-Aug-2019
Copyright: ©2019 da Silva Trevizan AC, et al. This is an open access paper distributed under the Creative Commons Attribution License.Journal of Health and Medical Research is published by Lexis Publisher.