Case Report - (2025) Volume 11, Issue 3
Background
Patients with multiple liver metastases from breast cancer are typically considered ineligible for surgical treatment due to the extent of disease. However, aggressive surgical strategies may offer long-term survival benefits in selected cases. This case series aims to illustrate the potential role of tailored surgical interventions in patients with extensive liver metastases.
Methods
We present two cases of female patients diagnosed with multiple bilobar liver metastases from breast cancer. The first patient, treated in 2020, had 20 bilobar liver metastases and underwent combined resection and radiofrequency ablation (RFA). The second patient, treated in 2023, had 18 bilobar metastases and underwent a two-stage hepatectomy using the associating liver partition and portal vein ligation for staged hepatectomy (ALPPS) procedure.
Results
Both patients achieved complete resection of all visible liver metastases through the respective surgical approaches. Follow-up assessments revealed no evidence of disease recurrence in either patient.
Conclusion
These cases demonstrate that, in carefully selected patients, aggressive and individualized surgical strategies may enable complete resection and provide the possibility of long-term survival, even in the setting of extensive liver metastases from breast cancer.
Breast cancer, Liver metastasis, Hepatectomy, ALPPS.
ALPPS: Associating Liver Partition and Portal vein ligation for Staged hepatectomy
BCLM: Breast Cancer Liver Metastasis
DFS: Disease-Free Survival
ER: Estrogen Receptor
HER2: Human Epidermal Growth Factor Receptor 2
HR: Hormone Receptor
PR: Progesterone Receptor
RFA: Radiofrequency Ablation
Liver metastasis is a common and devastating complication of breast cancer. Liver metastasis is a frequent and severe manifestation of advanced breast cancer, occurring in up to 50% of patients with metastatic disease. The presence of hepatic metastases, particularly when multiple and bilobar, is associated with poor prognosis and limited treatment options. Studies have reported a median overall survival of less than 2 years for patients with untreated breast cancer liver metastases (BCLM), underscoring the need for more effective interventions [1].
Traditionally, systemic chemotherapy has been the mainstay of treatment; however, its effectiveness is often limited in cases of extensive hepatic involvement. The objective response rates to chemotherapy in BCLM are generally modest, and durable control is rarely achieved in patients with a high tumor burden [2]. In recent years, advances in surgical techniques and perioperative management have expanded the therapeutic landscape. Emerging strategies such as staged hepatectomy, portal vein embolization (PVE), and local ablative therapies including radiofrequency ablation (RFA) have shown promise in improving resectability and long-term survival in select patients [3, 4].
Despite these advancements, the role of hepatic resection in BCLM remains controversial. Concerns persist regarding the aggressive tumor biology of metastatic breast cancer, high recurrence rates following resection, and the historically perceived lack of survival benefit. However, accumulating evidence suggests that in well-selected patients with good performance status and limited extrahepatic disease, aggressive surgical approaches may lead to significant survival gains. Several retrospective studies have demonstrated 5-year survival rates exceeding 30% in selected cohorts undergoing liver resection for BCLM [5, 6].
This case series presents two patients with multiple, bilobar liver metastases from breast cancer who underwent successful surgical management, including staged hepatectomy and local ablation. Their favorable outcomes underscore the importance of a multidisciplinary approach and suggest that aggressive, individualized surgical strategies can play a critical role in the management of complex hepatic metastases from breast cancer. [7].
Case 1
A 55-year-old female patient presented in January 2020 with 20 liver metastases (11 in the left lobe and 9 in the right lobe) (Figure 1). Previously, she was diagnosed with right-sided breast cancer with multiple life-threatening hepatic metastases in a local clinic. The patient was treated with palliative chemotherapy consisting of docetaxel and doxorubicin followed by tamoxifen, which blocks the effects of estrogen on hormone receptor-positive breast cancer. However, the disease progressed. She was referred to our surgery center and underwent a left lateral sectionectomy, partial resection of segment IV, multiple wedge resections of the right lobe, and intraoperative Radiofrequency Ablation (RFA) to ablate any remaining lesions (Figure 2, 3). The resected breast cancer cells were ER-positive, PR-negative and HER2-negative, and since then, we administered palbociclib with fulvestrant from May 14th 2020, to the present day for 5 years without recurrence (Figure 4).
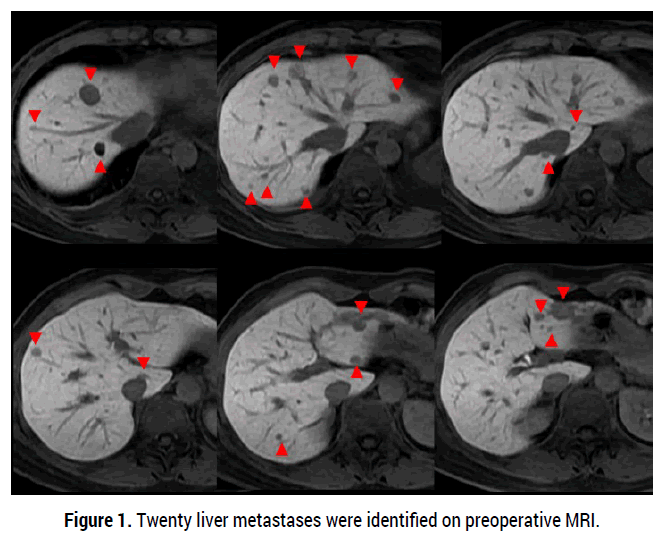
Figure 1. Twenty liver metastases were identified on preoperative MRI.
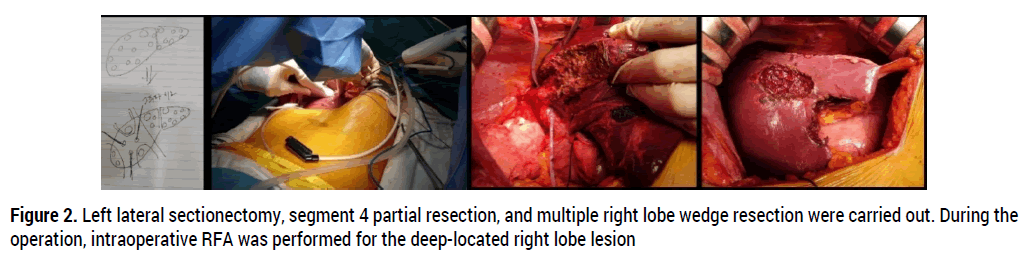
Figure 2. Left lateral sectionectomy, segment 4 partial resection, and multiple right lobe wedge resection were carried out. During the operation, intraoperative RFA was performed for the deep-located right lobe lesion.
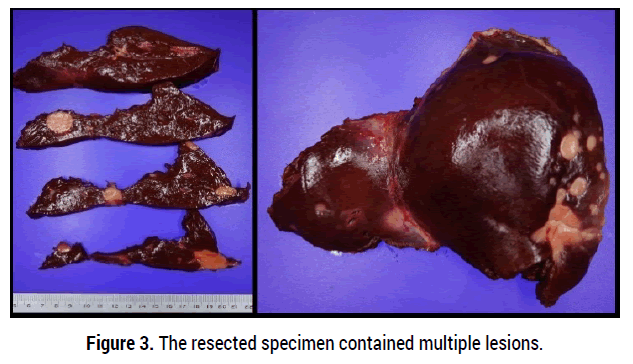
Figure 3. The resected specimen contained multiple lesions.
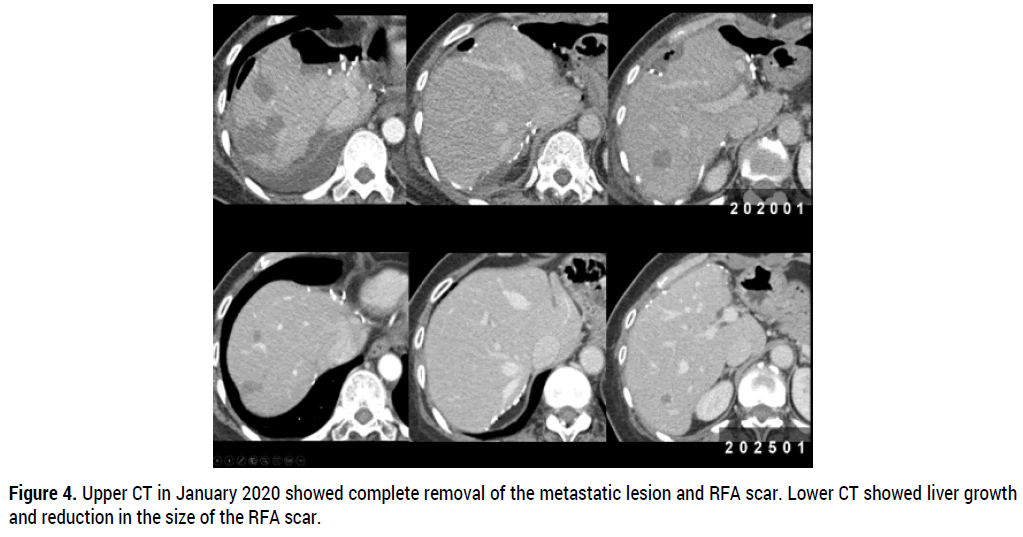
Figure 4. Upper CT in January 2020 showed complete removal of the metastatic lesion and RFA scar. Lower CT showed liver growth and reduction in the size of the RFA scar.
Case 2
• A 57-year-old female patient with pathologically confirmed triple negative left breast cancer presented with multiple liver metastases in November 2023 (Figure 5). At that time, she also had multiple bony metastases in the C3, T3, T11, L2 spines and right ilium.
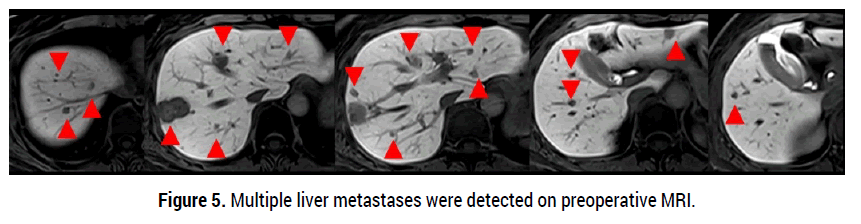
Figure 5. Multiple liver metastases were detected on preoperative MRI.
• Previously, the patient started chemotherapy with epirubicin plus docetaxel from December 2020 to May 2021 and subsequently underwent palliative breast-conserving surgery of a primary tumor sized 1.7 cm and concurrently removing metastatic lymph nodes in the local clinic. Additional paclitaxel was administered between April 2021 and October 2023. Unexpectedly, bony metastases in C3, T3, T11, L2 spines and right ilium were no longer seen on PET-CT on November 9th 2023. Thus, we performed a multidisciplinary committee and decided to perform liver resection.
• The patient underwent a two-stage hepatectomy using the ALPPS procedure. The first stage (November 20, 2023) involved multiple wedge resections of the left lobe, division of the left and right lobes, and ligation of the portal vein of the right lobe. The second stage (December 4, 2023) consisted of right hepatectomy (Figure 6). After curative surgery, we continued adjuvant chemotherapy with capecitabine plus vinorelbine over 12 times and finally achieved complete remission of the tumor (Figure 7).

Figure 6. The two images above show multiple metastatic lesions throughout the liver. The image on the lower left shows identification and the right hepatic artery and right portal vein. The image on the lower right shows multiple wedge resections of the left lobe lesion, division of the left and right lobes, and ligation and transection of the right portal vein.
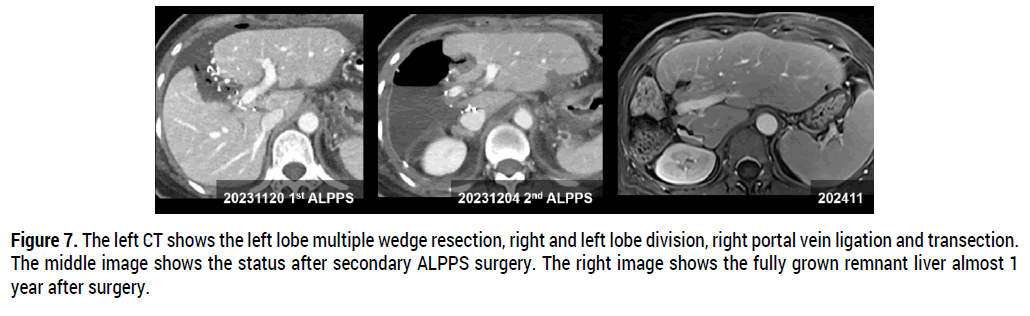
Figure 7. The left CT shows the left lobe multiple wedge resection, right and left lobe division, right portal vein ligation and transection. The middle image shows the status after secondary ALPPS surgery. The right image shows the fully grown remnant liver almost 1 year after surgery.
Breast cancer liver metastases (BCLM) have poor prognosis. Surgical resection is not the standard treatment and its suitability varies widely. The lack of clear guidelines for patient selection has led to inconsistent clinical practices [1]. Studies have shown a wide range of 5-year survival rates (9-78%) due to inconsistent eligibility criteria [2].
Several studies have shown that positive axillary lymph node involvement in breast cancer (BC) at the time of primary tumor resection is associated with poor outcomes. Patients with lymph node metastasis exhibited lower survival rates after resection for BCLM than those without nodal spread. [3, 4] This suggests that positive lymph nodes may indicate a more aggressive disease with the potential for occult micrometastases present even at the time of initial breast surgery [5] and [6].
Federica et al. demonstrated that patients with ER-positive primary tumors undergoing liver resection for BCLM exhibit better survival than those with ER-negative (including triple-negative) tumors [8]. This highlights triple-negative status as an independent poor prognostic factor for BCLM. These findings suggest that a selective approach to BCLM resection, considering both the receptor status and lymph node involvement of the primary tumor, should be adopted, even though the receptor status of the BCLM itself may differ [9, 10].
In addition, several prognostic factors appear to be related to the characteristics of the liver metastases, including the number, size, distribution, extent and radicality of liver resection. Patients with multiple BCLMs have a shorter median disease-free survival (DFS) than patients with a single metastasis, which is consistent with the results of this meta-analysis [9] and [10]. However, in our cases, good results were achieved despite the presence of multiple bilateral metastases of breast cancer (the first case had 20 lesions and the second case had 18 lesions).
Studies have demonstrated decreased overall survival (OS) and disease-free survival (DFS) in patients with BCLM larger than 30 mm (p = 0.041) or 40 mm. Several authors have proposed the use of tumor size as a criterion for selecting suitable candidates for surgical resection [5].
Federica et al. confirmed that a short interval between breast cancer diagnosis and the development of liver metastasis (BCLM) is an unfavorable prognostic factor. Previous studies have similarly demonstrated that patients undergoing liver resection may have worse outcomes when the interval between BCLM diagnosis and primary tumor treatment is less than 24 months [11, 12].
Their results also highlight the important role of curative surgery in achieving long-term survival. This importance extends beyond the absence of macroscopic residual disease, as described by Adam et al. in 2006, to the presence of microscopic residual disease [13]. A German study further supported this notion by identifying R1 resection (microscopic residual disease) as an independent prognostic factor for poor survival in multivariate analysis. The possibility of successful repeat liver resection in combination with systemic therapy, even in the presence of residual or recurrent disease, emphasizes the importance of achieving radical initial resection [14]. In our series, we performed radical R0 resection in both cases, and even performed RFA in three locations on the deep lesion in the first case to increase the curative rate. As a result, it seems to have shown a good prognosis.
Liver metastases are rarely the sole site of metastatic breast cancer. Therefore, many case series have included patients with BCLM and extrahepatic metastases, especially those with limited or well-controlled disease who responded to adjuvant chemotherapy. This has broadened the criteria for eligibility for resection. For example, Mariani et al. included patients with bone metastases, but did not explicitly exclude them as contraindications to surgery [15]. However, a previous study by Sakamoto et al. found that the presence of extrahepatic disease before liver resection was the only significant prognostic factor for poor outcome in multivariable analysis. Therefore, strict tumor surveillance after primary breast cancer treatment is essential for identifying patients with isolated liver metastases who may benefit from surgical resection [16]. In our second case, the patient underwent therapeutic ALPPS procedure after resolution of bone metastases, despite the presence of concomitant bone metastases.
As mentioned earlier, postoperative therapy following resection for BCLM and the presence of hormonal receptor status are among the most important factors affecting the long-term outcomes of patients with breast cancer because patients presenting with positive ER or PR seem to have the best long-term disease-free and overall survival [17]. As you seen in case 1, endocrine therapy is the preferred first-line treatment option for hormone receptor (HR)-positive and human epidermal growth factor receptor 2 (HER2)-negative metastatic breast cancer (MBC). Currently, a potent oral inhibitor of cyclin-dependent kinases (CDK) 4/6 in conjunction with fulvestrant is a novel therapeutic option for the treatment of HR-positive/HER2-negative MBC [18].
According to the PALOMA-3 study, a multicenter, randomized, double-blind, placebo-controlled, phase III trial was designed to assess the superiority of palbociclib in combination with fulvestrant compared with fulvestrant in prolonging PFS in women with HR-positive/HER2-negative MBC and disease progression after endocrine therapy. The primary endpoint was PFS, and the secondary endpoints included a comparison of safety between the treatment arms. The median progression-free survival was 9.2 months (95% confidence interval [CI], 7.5 to not estimable) with palbociclib–fulvestrant and 3.8 months (95% CI, 3.5 to 5.5) with placebo–fulvestrant (hazard ratio for disease progression or death, 0.42; 95% CI, 0.32 to 0.56; P<0.001) [19]. The emphasis here is on, in this report, the case 1 patient has survived over 5 years although she has received the same treatment with palbociclib–fulvestrant after surgical curative surgery for BCLM, which is superior to the median progression-free survival of the PALOMA-3 study. Therefore, successful metastasectomy to remove macroscopic or microscopic residual disease in patients with hepatic metastasis from primary breast cancer is critical [8].
By the way, the case 2 patient had triple negative left breast cancer with multiple liver metastases and had also multiple bony metastases in C3, T3, T11, La2 spines and right ilium at the time of diagnosis. The patient had her primary breast cancer removed and underwent chemotherapy at a nearby hospital. In general, patients with breast cancer with bone metastases rarely have their primary breast cancer removed. She received epirubicin and docetaxel [20] after mastectomy, but due to worsening of the disease, she received paclitaxel as a second-line drug for a relatively long period of time. In recent years, a combination of pembrolizumab, an immune checkpoint inhibitor and paclitaxel has become the standard treatment for triple-negative metastatic breast cancer. In the KEYNOTE-355 study, pembrolizumab-chemotherapy showed a significant and clinically meaningful improvement in progression-free survival compared to placebo-chemotherapy among patients with metastatic triple-negative breast cancer with a PD-L1 combined positive score (CPS) of 10 or more. These findings suggest a role for the addition of pembrolizumab to standard chemotherapy as first-line treatment for metastatic triple-negative breast cancer [21]. Nevertheless, since 2020, pembrolizumab has not been covered by insurance in Korea, so it is difficult to use it in practice.
This case series demonstrates the feasibility and potential efficacy of aggressive surgical approaches, including combined resection and RFA, and the ALPPS procedure, for managing multiple bilobar liver metastases from breast cancer. The successful outcomes in these two patients, with extended disease-free survival, highlight the importance of careful patient selection, meticulous surgical techniques, and a multidisciplinary approach. In particular, the ALPPS procedure offers a valuable option for patients with a limited FLR. [3].
Aggressive surgical strategies, tailored to individual patient characteristics, can offer significant benefits for highly selected patients with multiple liver metastases from breast cancer. Further studies with larger patient cohorts are needed to validate these findings and define optimal treatment algorithms.
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
, Manuscript No. 166725; , Pre QC No. 166725; , QC No. 166725; , Manuscript No. 166725; Published: 21-Jul-2025, DOI: 10.37532/24.11.3.1-4
Copyright:This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.