Case Reports - (2022) Volume 3, Issue 1
91-years-old male, with a history of atopic dermatitis and cerebrovascular disorder without sequelae. 7 months ago, he presented an erythematous plaque on the posterior chest, itching, with partial improvement for treatment. 2 months ago, the lesion increased in size with ulceration. He also presented other ulcers in the facial region, receiving antibiotic treatment with slight improvement. 1 month ago, new multiple ulcers were associated with a predominance of the scalp and anterior chest. 1 week ago, he went to the emergency for nasal obstruction and epistaxis. In the histopathological study of the skin, chronic granulomatous nodular dermatitis was evidenced. Stains were made with Schiff's periodic acid and Gomori-Grocott silver methenamine observing the presence of spherical structures compatible with Cryptococco skin sample culture confirms neoforman cryptococco infection. The presentation of this case is the atypical cutaneous manifestation such as multiple ulcers without systemic symptoms as the initial manifestation of disseminated cryptococcosis.
Cryptococcus • Disseminated cryptococcosis • Neoformans cryptococcus
Cryptococcosis is a fungal infection most frequently caused by cryptococcal neoformans, predominantly affecting immunocompromised individuals [1]. The clinical findings associated with cryptococcosis are frequently to lung and neurological diseases, but can also spread to the skin, joints, prostate, and eyeball [2]. The cutaneous involvement usually occurs in the course of disseminated mycosis and may precede other serious manifestations. It may present as papules, pustules, nodules, abscesses, edema, panniculitis, ulcers, similar to cellulite and molluscum contagiosum [3]. The diagnosis is based on mycological and histopathological examination [4]. Early treatment is important to decrease mortality in these patients [5].
We report the case of a male patient with multiple ulcers as an initial presentation of systemic cryptococcosis.
91-year-old male patient, with a history of atopic dermatitis and cerebrovascular disorder without sequelae presented 7 months ago, erythematous plaque on the posterior chest, itching, not painful with the histopathological study of spongy vesicular dermatitis, treatment with topical corticosteroids and antihistamines with partial improvement is indicated. Two months ago, the lesion increased in size with ulceration (Figure 1), and he also presented other ulcers in the facial region with antibiotic treatment with slight improvement. One month ago, new multiple ulcers appeared, predominantly on the scalp and anterior thorax (Figure 2). One week ago he went to the emergency for nasal obstruction and epistaxis so he was hospitalized.

Figure 1: Posterior trunk region, an ulcerated plaque with erythematous border, with seropurulent, painful discharge.
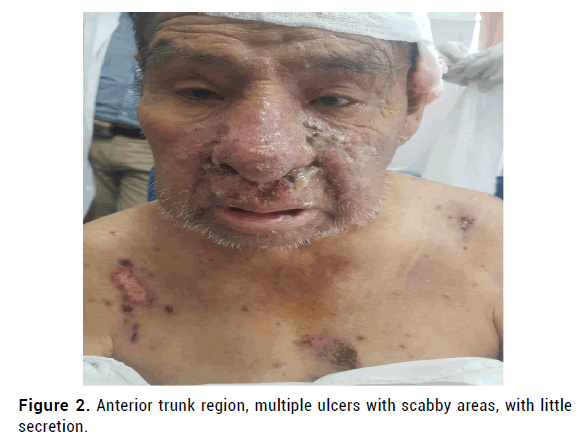
Figure 2: Anterior trunk region, multiple ulcers with scabby areas, with little secretion.
On physical examination, multiple ulcers predominantly on the trunk, scalp and facial region associated with the purulent discharge with hemorrhagic crusts in the nasal passages, submaxillary, cervical and inguinal lymphadenopathy, no respiratory symptoms or fever.
Laboratory tests: Leukocytes without neutrophilia (9.78 × 109/l, neutrophils 62%) creatinine: 0.73 mg/dL (0.5 mg/dL\-0.8 mg/dL), glucose: 81 mg/dL (74 mg/d/L-106 mg/d/L ), urea: 32.1 mg/dL (15 mg/dL-45 mg/ dL), FA: 648, TGO: 78 U/L (0-34 U/L), TGP: 59 U/L (13 U/L-69 U/L), GGTP: 421U/L (12 U/L-43 U/L), albumin: 2.4 mg/dL (3.2 mg/dL-4.8 mg/dL), DHL: 1075 U/L (50 U/L-150 U/L), globular sedimentation rate: 31 mm/h (<20 mm/h), C-reactive protein: 340.2 mg/L (<10 mg/L), coagulation profile: unaltered, serology for HIV antibodies: negative.
The following findings were observed in imaging techniques: chest radiograph with radiopaque infiltrates in the mid and basal fields (Figure 3) and multislice tomography of facial mass with pansinusitis predominantly bilateral ethmoid with thickening of the nasal mucosa, multiple lymphadenopathies in the pathological range with the appearance of secondary infiltration (Figure 4) computed tomography of the chest, abdomen and pelvis with multiple axillary, mediastinal, inguinal lymphadenopathy and interstitial lung infiltrate. Fine needle aspiration biopsy of inguinal adenopathy shows reactive lymphoid hyperplasia.

Figure 3: Chest X-ray A-P diffuses interstitial infiltrate predominantly in the middle and basal lung fields.

Figure 4: Multislice tomography of the facial mass-pansinusitis, multiple adenopathies of bilateral distribution in the parotid region, submaxillary and cervical.
Empirical antibiotic treatment with ceftriaxone and vancomycin was indicated, with no improvement in skin lesions. The clinical evolution was unfavourable, the patient presented a greater nasal discharge, respiratory distress and fever; nervous system involvement is not evident. Laboratory examinations and images were carried out with suggestive results of inhospital pneumonia for which he is referred to the pulmonology service; the patient died 2 days later.
On the histopathological study of skin biopsy: ulceration, chronic granulomatous nodular dermatitis with neutrophils, lymphocytes. Periodic acid Schiff staining and Gomori-Grocott silver methenamine are performed and spherical structures were observed, compatible with Cryptococcal infection (Figure 5). The culture of the skin sample confirms infection by cryptococcal neoformans. Subsequently, the result of the culture of the bronchial aspirate with the presence of cryptococcal neoformans was obtained.

Figure 5: Histopathological study of skin biopsy a) Chronic granulomatous nodular dermatitis (10x) b) Periodic acid Schiff stain with multiple oval spherical structures (10x) c) Gomori-Grocott silver methenamine staining, staining of the cell walls of the fungi is obse rved, suggestive of infection by cryptococci (10x).
Skin involvement in disseminated cryptococcosis may be an initial manifestation of disseminated infection [6].
Skin lesions may present as umbilicated, nodular, acneiform, herpetiform, cellulite, multiple ulcers, which can affect exposed and unexposed areas in some cases including without systemic signs and symptoms [7-9]. Our patient presented multiple ulcers, without neurological or respiratory symptoms of onset.
The spread of infection by cryptococcosis is rare in immunocompetent patients, the most frequent form of admission is by inhalation of spores causing pulmonary infection, which can remain localized and resolve spontaneously or spread to the central nervous system in immunocompromised patients; cutaneous involvement occurs more frequently in disseminated infection [10]. Our patient did not have proven immunosuppression.
The diagnosis of cryptococcosis can be made by histopathology of infected tissue, direct detection of fungi in body fluids with Indian ink examination, isolation in tissue culture and detection of cryptococcal polysaccharide antigen in serum and cerebrospinal fluid by agglutination by latex or ELISA. The patient case evidenced the presence of cryptococci in the histology, direct detection and culture of the skin sample. Current treatment recommendations suggest liposomal amphotericin B or amphotericin deoxycholate plus flucytosine for at least 14 days or until blood and cerebrospinal fluid cultures become sterile, in cases of patients with disseminated disease or systemic nervous system involvement. Our patient receives antibiotics on admission, later specific treatment for cryptococcosis is decided, but dies two days after diagnosis. Recognition of skin lesions due to cryptococcal infection is a great challenge since we can find clinical variability and therefore a delay in diagnosis with increased morbidity and mortality in these patients.
Authorship Contributions
The authors participate in the conception of the article; we participate in its drafting and the revision of the final version for publicationipate in its drafting and the revision of the final version for publication.
Conflict of Interest
The author report has no declarations of interest.
Citation: Coras N, et al. Polymorphic Skin Ulcers as Initial Manifestation of a Systemic Cryptococosis. Plast Surg: Case Studies. 2022, 3 (1), 001-003
Received: 08-Feb-2022 Published: 20-Feb-2022, DOI: 10.37532/pscs.22.3.1.1-3
Copyright: 2022 Coras N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.